Uncategorized
ASPN Committee Reports for Council 2024
Weekly Policy Update – March 1, 2024
 Thank you for your interest in accessing our exclusive content. Please note that this section is reserved for ASPN members only. If you're already a member, please log in using your credentials to unlock access using the button below. If you're not yet a member or if your membership has expired, don't worry! You can easily sign up or renew your membership to gain immediate access to all our valuable resources and benefits. To sign up or renew your membership, simply click here "Sign Up" or "Renew Membership", and follow the instructions. |
 |
Test
ASPN Council Candidate Request for Information
CTA showing renal artery stenosis
CTA showing right renal artery stenosis
Read MoreWilliam E. “Bill” Segar
Bill Segar died peacefully at home, in Indianapolis, IN on Feb 1, 2021. He was 97 years old. A very touching tribute to him was written by his son Jeff…
Read MoreJohn Herrin (2020)
It is with great sadness that we announce the passing on October 25, 2020 of John T. Herrin, MBBS, FRACP, 84, former Director of Clinical Services within the Division of Nephrology at Boston…
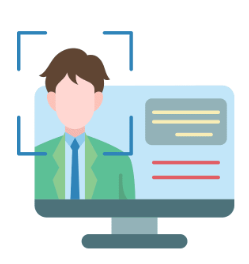
Read MoreSegmental glomerulosclerosis in IgA nephropathy
A patient with IgA nephropathy and associated segmental glomerulosclerosis. Images courtesy of Patrick Walker, MD.
Read MoreDivision Director’s Meeting
COVID-19 Resources
The PAS 2020 meeting has been cancelled due to the coronavirus pandemic. The PAS program office should communicate directly with you about hotel reservations (which should be automatically canceled if…
Read More